Bilateral pars defect2/29/2024 
Lumbosacral spondylolisthesis can be best assessed mainly on the lateral view, but occasional coronal deformity should not be missed. In cases where clinical examination indicates an abnormal sagittal balance of the spinal column, a whole spine lateral standing X-ray is indicated. In the majority of cases, an isthmic defect will be detected on radiographs but in doubtful cases. In severe L5/S1 slips, the L5 nerve root is most commonly affected by being pulled forward by the superior vertebra.įollowing the history and examination, the best screening tool is an AP and lateral weight-bearing X-ray of the lumbar spine. This situation is rare as most of the slips are only grade I or II, but the secondary canal and foraminal stenosis can occur due to subsequent degenerative changes in facet joints, hypertrophy of ligamentum flavum, hypertrophic fibrous repair tissue of the pars defect, or bulging of L5/S1 disc. Unlike the slip angle, the lumbosacral angle does not involve surfaces that alter with dysplasia.įorward translation of the vertebrae may cause a narrowing of the spinal canal at the level of the slip. The Dubosset’s lumbosacral angle is measured between the posterior aspect of the S1 and the upper endplate of the L5. It predicts intervention and affects cosmesis as well as prognosis. If slip angle measures >45 degrees, it is associated with a greater risk of slip progression, instability, and post-op pseudo-arthrosis. The Boxalls slip angle is measured between the perpendicular to the posterior aspect of the S1 vertebrae and the lower border of L5. The main parameters and their definitions are as follows.īoxall’s Slip Angle and Dubosset’s lumbosacral angle measures the relationship between L5 and S1. These parameters are measured on a standing lateral radiograph. The spinopelvic balance and the global spinal alignment are essential in understanding the etiology, grading, and planning the treatment protocol. In high-grade slips, the anterosuperior part of the sacrum becomes dome-shaped, which may be due to repeated trauma to the anterosuperior apophyseal ring of the S1 vertebrae. The repeated traction on the pars from a downsloping lumbosacral junction results in failure and fracture of the pars interarticularis. The second mechanism is when there is an increased sacral slope and hence increased traction on the pars interarticularis. This condition is more likely to occur in a situation where the sacral slope has a low value with a more horizontally orientated superior sacral endplate. The inferior facet of L4 and the superior facet of S1 creates a pincer effect on the pars interarticularis, causing a failure of the L5 pars. The first is the pincer effect due to repeated hyperextension. Two mechanisms may cause the lytic defect. Management of the majority of the cases is non-operative, but patients who fail non-operative treatment and continue having disabling symptoms may require surgical treatment. Presentation in adults is more insidious and commonly associated with long-standing degenerative changes secondary to the slip, often leading to spinal canal stenosis and radicular pain. Occasionally pain can radiate to both buttocks and legs, and in advanced cases, the gait pattern and walking distance may be affected. 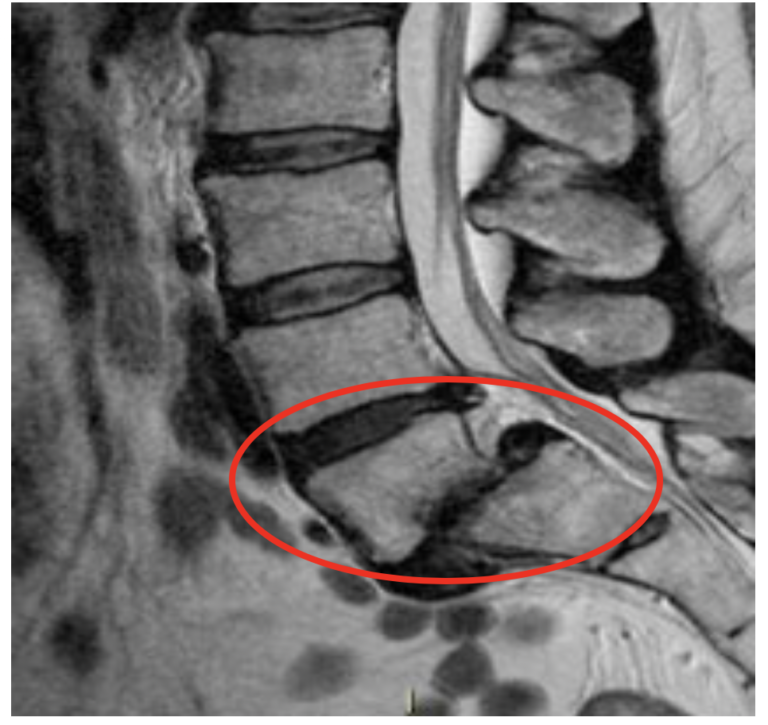
The most commonly affected populations are children and adolescents participating in sports that require repetitive lower back hyperextension (divers, pace cricket bowlers, baseball, softball, rugby, weightlifting, sailing, table tennis, wrestlers, gymnasts, dancers, and footballers). They usually present with lower back pain exacerbated by activity. The majority of cases are mild or asymptomatic, and only a relatively small percentage of symptomatic patients require surgical intervention. The prevalence of spondylolysis (pars defect), in the general population, is 6%, and a third of those will subsequently develop a degree of spondylolisthesis. The degree of a slip often correlates with the degree of symptoms. Bilateral L5 pars defect (spondylolysis) or repetitive stress injury is the primary etiology behind lumbosacral spondylolisthesis. Lumbosacral spondylolisthesis is the forward translation of the fifth lumbar vertebra (L5) over the first sacral vertebra (S1).
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
